Thumb Arthritis
Thumb Arthritis: Symptoms and Surgical Techniques
One of the most common causes of pain when pinching, grasping, torquing (twisting), and lifting with the hand, is arthritis at the base of the thumb. A complex saddle-shaped joint at the base of the thumb allows for movement of the thumb away from the palm. This joint also allows the thumb to pivot and turn so as to meet one or all of the fingers in opposition, which one might visualize as the thumb touching each of the fingertips. This complex function requires that the thumb be strong, flexible, and stable. The forces generated at the thumb base joint are extremely high. In a simple pinching maneuver, the force is 12 times greater at the base of the thumb than it is at the tip of the thumb. A lifetime of use, or trauma, may lead to osteoarthritis of this joint, the trapeziometacarpal joint, which is located between the trapezium and first metacarpal (see figure 1). Even the simplest tasks of daily living such as turning a key, grasping a doorknob, opening a car door, buttoning a shirt, or brushing ones’ teeth, can become impossible when one suffers from trapeziometacarpal joint arthritis.
Risk Factors for Thumb Arthritis
Osteoarthritis of this joint is most commonly seen in middle-age or postmenopausal women. Female prevalence of this degenerative process is most likely due to greater joint laxity which leads to increased joint incongruity (the two sides of the joint don’t line up smoothly and evenly). Combining joint incongruity with high frequent forces leads to an accelerated degenerative process (osteoarthritis).
Image of 3D Human Hand Anatomy
A careful clinical examination of the thumb and x-rays will make the diagnosis of osteoarthritis of the trapeziometacarpal joint. There are many treatments for trapeziometacarpal joint arthritis. Rest and non-steroidal anti-inflammatory medications should be the first step. If this fails, the treating physician may wish to try a Medrol Dosepak and consider a custom designed splint for the hand and thumb. An occupational therapist with special splint training will make a hand base splint that incorporates the thumb. Unfortunately, most patients have difficulty tolerating the splint. It reduces thumb function considerably by limiting mobility of the trapeziometacarpal joint. Another option is an injection of corticosteroid into the trapeziometacarpal joint. The injection will usually resolve the pain in the early stages of arthritis; advanced stages may have no improvement. If there is no improvement in pain despite the conservative efforts, the next step would be to consider surgical intervention.
Surgery for the Thumb
The development of this new surgical technique has a design is to last a lifetime. In this surgery, there is a removal of the arthritis at the base of the thumb. (see figure 2). An extra wrist flexor tendon, the flexor carpi radialis tendon, is released in the mid-forearm and placed through the bone at the base of the thumb (see figure 3). It is secured under tension to the base of the thumb by using a suture arising from an anchor. The surgeon then channels this tendon underneath the base of the thumb and weaves it back and forth to itself. This fills the space where the arthritis bone once was. Because the blood supply to the tendon remains the same, this living joint replacement tissue becomes stronger with time. This surgical procedure takes less than an hour to complete in an outpatient setting. Therapy will start after 10 days and the protective splint is worn for 6 weeks following surgery. Long-term follow up studies have shown 95% of patients experiencing excellent relief of pain while also restoring thumb function.
.jpg)
Image of the Hand
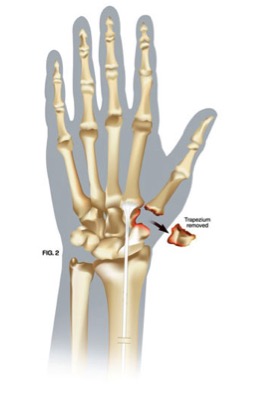
Hand trapezium removed.
JOI and JOI Rehab
JOI Physicians continue to offer online new patient appointments. This is another option to make it more convenient to make new patient appointments with less phone hold times. Follow the link below to select your JOI MD and schedule online.
You can still call 904-JOI-2000 to make new patient JOI Physician Appointments if that is your preference.
To make appointments with JOI Rehab, please call 904-858-7045.