ACL Recovery
By Dr. Kevin Kaplan
Dr. Kaplan ACL & ACL Recovery
One of the most common injuries I see in my office is a tear of the anterior cruciate ligament (ACL). Most of these injuries occur during a rapid change in direction, landing from a jump, pivoting, or from contact to the knee during activities (ex: tackling in football). Other high-risk sports include soccer, skiing, and basketball.
Most patients describe the sensation or the sound of a pop in the knee followed by difficulty ambulating and swelling. In addition, patients may describe the feeling of instability or buckling in the knee after tearing an ACL. To read more about this subject, please read Torn ACL Symptoms.
Figure 1: Anatomy of the Knee
Figure 2: MRI – ACL Tear
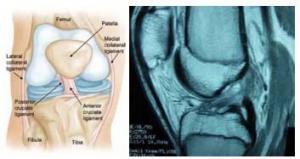
Image of the ACL and MRI
What is the ACL?
So, what is the ACL and why is it so important to an active patient? The anterior cruciate ligament connects the femur (thigh bone) to the tibia (shin bone) (figure one). It is one of four main ligaments providing stability to the knee joint. The ACL prevents excessive forward motion of the tibia in relation to the femur. It also prevents excessive rotation of the knee joint.
By examining the knee, I can evaluate the ACL in addition to the other ligaments and cartilage in the knee. The Lachman test and anterior drawer test are the two best exams for determining the integrity of the ACL.
In order to obtain a definitive diagnosis, patients are usually led to have an MRI (magnetic resonance imaging). An MRI evaluates the soft tissue structures and will provide information about the cartilage and ligaments in the knee (Figure two).
Unfortunately, given the fact that the ACL is located within the knee joint and is surrounded by joint fluid, it does not
have the ability to heal once it’s torn. The options after being diagnosed with an ACL tear are conservative management with bracing the knee in combination with rehabilitation or operative management with an ACL reconstruction.
Non-operative Approach to ACL Injuries
Treatment is for individuals who do not have symptoms of instability and do not plan on returning to high-level activities.
Inactive, healthy patients with the desire to continue activities requiring cutting and pivoting, my recommendation is to reconstruct the ACL2. Reconstructing the ACL involves substituting a tendon in the location of t
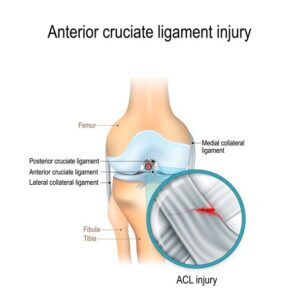
ACL tear
e patient’s original ligament. This tendon then becomes the new ligament over a period of several months. The tendons used for reconstruction can be obtained from the patient (autograft) or can be obtained from cadaveric tissue (allograft).
Recent orthopaedic studies have shown greater than 20% failure rates when using allograft in patients younger than 253. Thus, in my practice, I strongly recommend autograft in this patient demographic. Patients older than 25 are given the options to have autograft versus allograft after a thorough discussion of all of the potential risks, benefits, and alternatives.
The two most commonly utilized autografts include the patellar tendon and the hamstring tendon. Both have shown similar high success rates in returning patients to an active lifestyle.
JOI Journal
Regardless of graft choice, ACL reconstruction is done on an outpatient basis and typically takes one to two hours to perform depending on if there is any other concomitant cartilage injury in the knee. With the aid of a camera and through small incisions in the skin, the new ACL goes into the knee through tunnels in the femur and tibia and metal or bioabsorbable screws stabilize the graft in these tunnels
Rehabilitation begins immediately with a focus on obtaining full knee extension and working on strengthening the muscles surrounding the knee. Patients utilize an extension brace and crutches for support in the early postoperative period. The process of the new graft becoming a ligament takes several months to occur. During this period of ligamentization, the patient will be working on range of motion, strength, and agility training. Typically, running doesn’t begin until 4 months postoperatively and a clearance to full sport occurs at 9 months.
ACL Reconstructions
I would like to finish up by answering common questions that I hear in my office in regard to ACL reconstructions. What is the success rate of this operation? The rate of success in creating a stable knee is between 85-90%. Over the last 10 years, we have focused on a more anatomic reconstruction of the ACL in attempts to decrease any potential failures. Can I re-tear my ACL? The new ACL (if allowed to gain it’s full strength over the rehabilitation period) can tear again, but should be at as much of a risk to tear as your native ACL. Am I going to get arthritis in the future?
There is a chance given the injury and also if there is meniscus or cartilage damage at the time of injury that the knee may get arthritis in the future, but this is unpredictable. How can I put myself at risk for a re-tear after the surgery? Most patients feel comfortable and pain-free after the first few months. However, what we know biologically is that the ACL graft does not incorporate and become a new ligament for quite some time. Trying to rush back to sports is one of the main reasons why athletes sustain early re-tears.
ACL injuries are devastating to both professional and recreational athletes. However, surgical reconstruction of this important stabilizing ligament has a high rate of success in allowing patients to return to their desired sport.
References
1. Griffin LY. Noncontact Anterior Cruciate Ligament Injuries: Risk Factors and Prevention Strategies. J Am Acad Orthop Surg 2000;8:141-150.
2. Johnson RJ, Beynnon BD, Nichols CE, et al. Current concepts review. The treatment of injuries of the anterior cruciate ligament. J Bone Joint SurgAm 1992;74A:140-151.
3. Sun K, Tian S, Zhang J, Xia C, Zhang C, Yu T. Anterior cruciate ligament reconstruction with BPTB autograft, irradiated versus non- irradiated allograft: a prospective randomized clinical study. Knee Surg sports Traumatol Arthrosc 2009;17(5):464-74.
Related Article:
If you are interested in scheduling an appointment at JOI Rehab for physical therapy, call (904) 858-7045. Come see us!
JOI and JOI Rehab
JOI Physicians continue to offer online new patient appointments. Make an appointment by calling (904) JOI-2000 or schedule online. This is a new option to make it more convenient to make new patient appointments. Follow the link below to select your JOI MD and schedule online.